Colorectal cancer is the third most common type of non-skin cancer in both men (after prostate cancer and lung cancer) and women (after breast cancer and lung cancer). It is the second leading cause of cancer death in the United States after lung cancer. Although the rate of new colorectal cancer cases and deaths is decreasing in this country, more than 145,000 new cases were diagnosed and more than 49,000 people died from this disease each year over the past 5 years.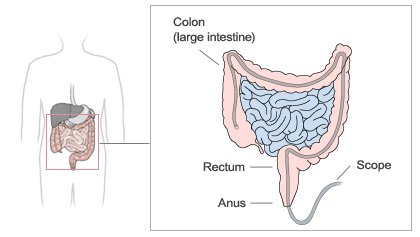
The exact causes of colorectal cancer are not known. However, studies have shown that certain factors are linked to an increased chance of developing this disease, including the following:
Age
Colorectal cancer is more likely to occur as people get older. Although this disease can occur at any age, most people who develop colorectal cancer are over age 50.
Polyps
Polyps are abnormal growths that protrude from the inner wall of the colon or rectum. They are relatively common in people over age 50. Detecting and removing these growths may help prevent colorectal cancer.
Personal History
A person who has already had colorectal cancer is at an increased risk of developing colorectal cancer a second time. Some women with a history of ovarian, uterine, or breast cancer have a higher than average chance of developing colorectal cancer.
Family History
Close relatives (parents, siblings, or children) of a person who has had colorectal cancer are somewhat more likely to develop this type of cancer themselves, especially if the family member developed the cancer at a young age.
Ulcerative Colitis or Crohn’s Colitis
People who have ulcerative colitis or Crohn’s colitis are more likely to develop colorectal cancer than people who do not have these conditions.
Diet
Some evidence suggests that the development of colorectal cancer may be associated with high dietary consumption of red and processed meats and low consumption of whole grains, fruits, and vegetables.
Exercise
Some evidence suggests that obesity and a sedentary lifestyle is associated with an increased risk of developing colorectal cancer.
Smoking
Increasing evidence from epidemiologic studies suggests that cigarette smoking, particularly long-term smoking, increases the risk of colorectal cancer.
Screening and Its Importance
Screening is checking for health problems before they cause symptoms. Colorectal cancer screening can detect cancer, polyps, nonpolypoid lesions, (flat or slightly depressed areas of abnormal cell growth) and other conditions. Flat or depressed lesions occur less often than polyps, but they may have a greater potential to develop into colorectal cancer. Finding and removing polyps or other areas of abnormal cell growth is the most effective way to prevent colorectal cancer. Colorectal cancer (like most cancers) is generally more treatable when it is found early.
The following tests are available for colorectal cancer screening:
Colonoscopy
Virtual colonoscopy
Double contrast barium enema
Flexible Sigmoidoscopy
Fecal occult blood test (FOBT)
You should talk to your doctor about when to begin screening for colorectal cancer, which test to have, the benefits and risks of each test, and the frequency of testing.
Crohn’s disease is a chronic disorder that causes inflammation of the (GI) tract. Although it can involve any area of the GI tract from the mouth to the anus, it most commonly affects the small intestine and/or colon. Crohn’s and a related disease, ulcerative colitis, are the two main disease categories that belong to a larger group of illnesses called inflammatory bowel disease (IBD).
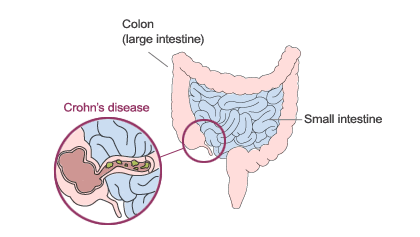
Because the symptoms of these two illnesses are so similar, it is sometimes difficult to establish the diagnosis definitively. Both illnesses do have one strong feature in common. They are marked by an abnormal response by the body’s immune system. In people with Crohn’s disease, the immune system reacts inappropriately. Researchers believe that the immune system mistakes microbes, such as bacteria that is normally found in the intestines, for foreign or invading substances, and launches an attack. In the process, the body sends white blood cells into the lining of the intestines, where they produce chronic inflammation. These cells then generate harmful products that ultimately lead to ulcerations and bowel injury.
We do not yet know what causes this disease. Studies indicate that the inflammation in Crohn’s disease involves a complex interaction of factors: the genes the person has inherited, the immune system, and something in the environment. Foreign substances (antigens) in the environment may be the direct cause of the inflammation, or they may stimulate the body’s defenses to produce an inflammation that continues without control. In patients with Crohn’s disease, once the patient’s immune system is “turned on,” it does not know how to properly “turn off.” As a result, inflammation damages the intestine and causes the symptoms of Crohn’s disease. One of the major goals of medical therapy is to help patients regulate their immune system better.
It is estimated that as many as one million Americans have IBD — with that number evenly split between Crohn’s disease and ulcerative colitis. Males and females appear to be affected equally. Crohn’s disease may occur in people of all ages, but it is primarily a disease of adolescents and young adults, affecting mainly those between the age of 15 and 35. However, it can also occur in people outside this age group.
IBD tends to run in families. Studies have shown that about 20 to 25 percent of patients may have a close relative with either Crohn’s or ulcerative colitis. If a person has a relative with the disease, his or her risk is about 10 times greater than that of the general population. If that relative happens to be a brother or sister, the risk is 30 times greater. There is no way to predict which, if any, family members will develop Crohn’s disease.
IBD is more commonly found in certain ethnic groups. American Jews of European descent are four to five times more likely to develop IBD than the general population. IBD has long been thought of as a disease predominantly affecting Caucasians. However, there has been a steady increase in reported cases of both Crohn’s disease and ulcerative colitis among African Americans. The prevalence rates among Hispanics and Asians are lower than those for Caucasians and African Americans.
Symptoms
Symptoms of Crohn’s disease include persistent diarrhea (loose, watery, or frequent bowel movements), crampy abdominal pain, fever, fatigue, and, at times, rectal bleeding. Symptoms vary from person to person and may change over time. Loss of appetite and subsequent weight loss also may occur. Of note is that the disease is not always limited to the GI tract; it can also affect the joints, eyes, skin, and liver. Some patients may develop tears (fissures) in the lining of the anus, which may cause pain and bleeding, especially during bowel movements. Chronic, severe inflammation may also cause a fistula to develop. A fistula is a tunnel that leads from one part of the intestine to another, or that connects the intestine to the bladder, vagina, or skin. Fistulas occur most commonly around the anal area. If this complication arises, you may notice drainage of mucus, pus, or stool from this opening.
Symptoms may range from mild to severe. Because Crohn’s is a chronic disease, patients may go through periods in which the disease flares up, when the disease is active. These episodes are often followed by times of remission, when the symptoms disappear or decrease. In general, people with Crohn’s disease lead full, active, and productive lives.
Diagnosing Crohn’s Disease
There is no single test that can confirm the diagnosis of Crohn’s disease. Doctors rely on a combination of the patient’s history and physical exam, results of laboratory tests, X-rays (small bowel series), colonoscopy and recently, small bowel capsule endoscopy. Crohn’s disease often mimics other conditions.
Medications Used to Treat Crohn’s Disease
Currently, there is no cure for Crohn’s disease. The goal of medical treatment, therefore, is to modulate the inflammatory response.
Several groups of drugs are used to treat Crohn’s disease today. They are:
1. Aminosalicylates (5-ASA): These medications typically are used to treat mild to moderate symptoms.
2. Corticosteroids: These drugs have significant short- and long-term side effects and should not be used as a maintenance medication.
3. Immune modifiers: Azathioprine (Imuran®), 6-MP (Purinethol®), and methotrexate are used to help decrease corticosteroid dosage and also to help heal fistulas. In addition, immune modifiers can help maintain disease remission.
4. Antibiotics: metronidazole, ciprofloxacin, rifaximin (Xifaxan®)
Biologic Therapies
Infliximab (Remicade®), adalimumab (Humira®), certolizumab pegol (Cimzia®), natalizumab (Tysabri®). These medications are used for inducing and maintaining clinical response and remission in adult patients with moderately to severely active Crohn’s disease who have had an inadequate response to, or are unable to tolerate, conventional Crohn’s disease therapies.
Role of Surgery
Two-thirds to three-quarters of patients with Crohn’s disease will require surgery at some point during their lives. Surgery becomes necessary in Crohn’s disease when medications can no longer control the symptoms. It may also be performed to repair a fistula or fissure. Another indication for surgery is the presence of an intestinal obstruction or other complication, such as an intestinal abscess. Surgery is not considered a cure for Crohn’s disease, because the disease frequently recurs at or near the site where the intestine has been reattached (anastomosis). The overall goal of surgery in Crohn’s disease is to conserve bowel and return the individual to the best possible quality of life.
Nutrition
There is no evidence that any particular foods cause or contribute to Crohn’s disease. Paying special attention to diet may help reduce symptoms, replace lost nutrients, and promote healing.
When Crohn’s disease is active, soft, bland foods may cause less discomfort than spicy or high-fiber foods. Except for restricting milk in lactose-intolerant patients, most gastroenterologists try to be flexible in planning the diets of their Crohn’s patients. A healthy diet should contain a variety of foods from all food groups. Meat, fish, poultry, and dairy products (if tolerated) are sources of protein; bread, cereal, starches, fruits, and vegetables are sources of carbohydrate; margarine and oils are sources of fat.
Emotional Factors
There is no evidence to show that stress, anxiety, or tension is responsible for Crohn’s disease. However, they may contribute to an exacerbation of the disease. Emotional distress that patients sometimes feel may be a reaction to the symptoms of the disease itself. Although formal psychotherapy is generally not necessary, some patients are helped considerably by speaking with a therapist who is knowledgeable about IBD or about chronic illness in general.
Ulcerative colitis is a chronic disease of the colon (large intestine). The disease is marked by inflammation and ulceration of the colon lining which makes the colon empty frequently. Symptoms include diarrhea (sometimes bloody) and often crampy abdominal pain. The inflammation usually begins in the rectum and lower colon, but it may also involve the entire colon. When ulcerative colitis affects only the rectum, it is called ulcerative proctitis.
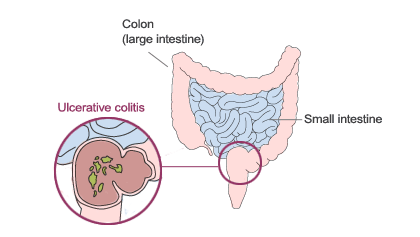
Ulcerative colitis differs from Crohn’s disease. Both diseases are called inflammatory bowel disease (IBD). Crohn’s disease can affect any part of the GI tract, whereas ulcerative colitis affects only the colon. The inflammation affects only the innermost lining of the colon, but in Crohn’s disease, it can affect the entire thickness. Inflammation from ulcerative colitis occurs in a continuous process – there are no areas of normal intestine between the areas of diseased intestine. In contrast, “skip” areas may occur in Crohn’s disease.
In inflammatory bowel disease, there is an abnormal response by the body’s immune system. Researchers believe that the immune system mistakes food, bacteria and other materials in the intestine for foreign or invading substances, and launches an attack. In the process, the body sends white blood cells into the lining of the intestines, where they produce chronic inflammation. These cells then generate harmful products that ultimately lead to ulcerations and bowel injury.
We do not yet know what causes this disease. Studies indicate that the inflammation in ulcerative colitis involves a complex interaction of factors: the genes the person has inherited, the immune system, and something in the environment. Foreign substances (antigens) in the environment may be the direct cause of the inflammation, or they may stimulate the body’s defenses to produce an inflammation that continues without control. In patients with ulcerative colitis, once the patient’s immune system is “turned on,” it does not know how to properly “turn off.” As a result, inflammation damages the intestine and causes the symptoms of ulcerative colitis. One of the major goals of medical therapy is to help patients to better regulate their immune system.
It is estimated that as many as one million Americans have IBD — with that number evenly split between Crohn’s disease and ulcerative colitis. Males and females appear to be affected equally. The usual age of diagnosis with ulcerative colitis is in the mid-30’s, although the disease can occur at any age. Men are more likely than women to be diagnosed with ulcerative colitis in their 50s and 60s. The incidence is greater in whites than non-whites, and a higher incidence is found in Jews than in non-Jews.
IBD tends to run in families. Studies have shown that up to 20 percent of patients with ulcerative colitis will have a close relative with either Crohn’s disease or ulcerative colitis. There is no way to predict which, if any, family members will develop ulcerative colitis.
Symptoms
Symptoms of ulcerative colitis include diarrhea (often bloody) which may be associated with crampy abdominal pain and sudden urgency to have a bowel movement. The diarrhea may begin slowly or quite suddenly. Loss of appetite, weight loss and fatigue are also common symptoms. In cases of severe bleeding, anemia may occur. Approximately half of all patients with ulcerative colitis have relatively mild symptoms. The symptoms of ulcerative colitis tend to come and go, with fairly long periods in between flare-ups in which patients may experience no distress at all. These periods of remission can span months or even years, although symptoms do eventually return. Of note is that the disease is not always limited to the GI tract; it can also affect the joints, eyes, skin, and liver.
Diagnosing Ulcerative Colitis
The diagnosis of ulcerative colitis is based on the patient’s clinical history, a physical exam and a series of tests which usually includes: stool studies, blood tests and a colonoscopy.
Medications Used to Treat Ulcerative Colitis
Currently, there is no cure for ulcerative colitis. The goal of medical treatment, therefore, is to modulate the inflammatory response.
Several groups of drugs are used to treat ulcerative colitis. They are:
1. Aminosalicylates (5-ASA): These medications typically are used to treat mild to moderate symptoms.
2. Corticosteroids: These drugs have significant short and long-term side effects and should not be used as a maintenance medication.
3. Immune modifiers: Azathioprine (Imuran®), 6-MP (Purinethol®), and methotrexate are used to help decrease corticosteroid dosage and also to help heal fistulas. In addition, immune modifiers can help maintain disease remission.
4. Antibiotics: metronidazole, ciprofloxacin, ampicillin, others.
5. Biologic therapies. Infliximab (Remicade®). Infliximab is used for people with moderate-to-severe ulcerative colitis.
Role of Surgery
In one-quarter to one-third of patients with ulcerative colitis, medical therapy is not completely successful or complications arise. Under these circumstances, surgery may be considered. This operation involves the removal of the colon (colectomy). Ulcerative colitis is “cured” once the colon is removed.
Nutrition
There is no evidence that any particular foods cause or contribute to ulcerative colitis. Paying special attention to diet may help reduce symptoms, replace lost nutrients, and promote healing. Maintaining proper nutrition is important for the medical management of ulcerative colitis.
Except for restricting milk in lactose-intolerant patients, or restricting coffee when severe diarrhea occurs, most gastroenterologists recommend a well balanced diet. A healthy diet should contain a variety of foods from all food groups. Meat, fish, poultry, and dairy products (if tolerated) are sources of protein; bread, cereal, starches, fruits, and vegetables are sources of carbohydrate; margarine and oils are sources of fat.
Emotional Factors
There is no evidence to show that stress, anxiety, or tension is responsible for ulcerative colitis. However, they may contribute to an exacerbation of the disease. Emotional distress that patients sometimes feel may be a reaction to the symptoms of the disease itself. Although formal psychotherapy is generally not necessary, some patients are helped considerably by speaking with a therapist who is knowledgeable about IBD or about chronic illness in general.
Diverticulosis refers to the presence of small out-pouchings (called diverticuli) or sacs that can develop in the lining of the gastrointestinal tract. While diverticuli can be present anywhere in the entire digestive tract, they are most common on the left side of the large intestine, the area known as the descending and sigmoid colon.
Diverticulosis is a common disorder especially in older people. The condition is rarely seen in people under the age of 30 and is most common in those over 60. Both men and women are equally affected.
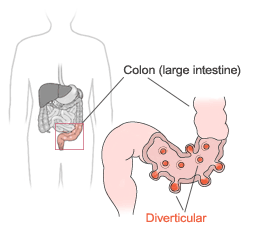
No one knows for certain why diverticulosis develops; however, a few theories have been suggested. Abnormal contraction and spasm (resulting in intermittent high pressure in the colon) may cause diverticula to form in a weak spot of the intestinal wall. Constipation leads to excess intra-colonic pressure and is thought to be responsible for some cases of diverticulosis. A diet rich in fiber (bran cereals, whole wheat breads, fresh fruits, and leafy vegetables) may decrease the development of diverticulosis, improve symptoms of constipation and decrease the likelihood of complications. Benefits of a high fiber diet may be seen in those who eat between 15 and 30grams of fiber a day. Unfortunately people in the United States generally only consume 8-12 grams a day. Diverticulosis does not appear to be associated with alcohol, smoking or caffeine consumption. There also appears to be a genetic predisposition. Once diverticuli have formed they do not go away.
Most patients with diverticulosis have no symptoms. Many will never know they have the condition until it is discovered during a colonoscopy or radiographic examination. While most people have no symptoms, some individuals may experience pain or discomfort in the abdomen, bloating, and/or a change in bowel habits.
Diverticulosis is generally discovered through one of the following examinations:
- Colonoscopy
- CT scan
- Barium enema
Diverticulitis is an inflammation and/or infection of one of the diverticula. People with this complication characteristically present with:
- Fever
- Abdominal pain, often on the lower left side
- Diarrhea and/or constipation
- Decreased appetite
Other complications of diverticulitis include development of an abscess or narrowing of the colon (stricture). In rare cases, a fistula or connection between the bowel and bladder may occur as a complication of diverticulitis.
Hemorrhage or the passage of large amount of bright red blood from the rectum is another potential complication. It occurs typically without warning and is painless. Severe bleeding has been reported in 3-5% of people with diverticulosis and usually stops without special treatment.
Treatment for diverticulitis (an inflamed or infected diverticulum) requires the use of antibiotics and occasionally hospitalization. Recovery is usually uneventful. Surgery is rarely required but may be needed for cases that don’t respond to medical management.
Individuals with diverticulosis are sometimes instructed to avoid foods that contain indigestible particles such as popcorn, nuts and fruits with small seeds. The theory is that these particles might get “stuck” in a diverticulum which may then lead to diverticulitis. While there is no objective evidence to support this recommendation, the latest research suggests that eating nuts may reduce the risk for diverticulitis in individuals with diverticulosis.
