Incidence:
More than 60 million Americans experience heartburn (acid indigestion) at least once a month and more than 15 million Americans experience heartburn symptoms each day.
Gastroesophageal Reflux
Gastroesophageal reflux is a physical condition in which acid from the stomach flows backward up into the esophagus. People can experience heartburn when excessive amounts of acid reflux into the esophagus.
Many describe heartburn as a burning discomfort, localized behind the breastbone that moves up toward the neck and throat. Some even experience the bitter or sour taste of the acid in the back of the throat or mouth. The burning and pressure symptoms of heartburn can last for several hours and often worsen after eating food. Occasional heartburn is very common. However, frequent heartburn, (two or more times a week), difficulty swallowing or weight loss may be associated with a more severe problem known as gastroesophageal reflux disease or GERD. Most people will experience heartburn if the lining of the esophagus comes in contact with too much stomach juice for too long a period of time. This stomach juice consists of acid, digestive enzymes, and other injurious materials. The prolonged contact of acidic stomach juice with the esophageal lining injures the esophagus and produces a burning discomfort. Normally, a muscular valve at the lower end of the esophagus called the lower esophageal sphincter (LES) keeps the acid in the stomach and out of the esophagus. In gastroesophageal reflux disease or GERD, the LES relaxes too frequently, which allows stomach acid to reflux, or flow backward into the esophagus.
>
Tests to evaluate for GERD
Upper Endoscopy
This test involves passing a thin flexible tube through the mouth into the esophagus, stomach and the beginning of the small bowel to examine for abnormalities. The tube has a light and a camera at the tip and the lining of digestive tract is directly visualized. The test is performed using sedation. It is the best test to identify injury (erosions and ulcers) in the upper GI tract and Barrett’s esophagus.
Upper GI Series
This test involves drinking a liquid barium mixture. The radiologist uses a fluoroscope to watch the barium as it travels down the esophagus and into the stomach. The patient is asked to move into various positions on the X-ray table while the radiologist watches the GI tract and takes X-rays.
Esophageal Manometry or Esophageal PH
Esophageal manometry involves passing a small flexible tube through the nose into the esophagus and stomach in order to measure pressures and function of the esophagus. The acid level in the esophagus can be measured over a 48-hour period by attaching a capsule to the lining of the esophagus.
Extra-Esophageal Manifestations (EEM): GERD can masquerade as other diseases
Increasingly, we are becoming aware that the irritation and damage to the esophagus from continual presence of acid can prompt an entire array of symptoms other than simple heartburn. The role of acid reflux has been overlooked as a potential factor in the diagnosis and treatment of patients with chronic cough, hoarseness and asthma-like symptoms. In some instances, patients have never reported heartburn.
Potential Complications from GERD
Peptic Stricture
This results from chronic acid injury and scarring of the lower esophagus. Patients complain of food sticking in the lower esophagus.
Barrett’s Esophagus
A serious complication of chronic GERD is Barrett’s esophagus. The lining of the esophagus, in patients with Barrett’s esophagus has changed to resemble the stomach lining. As a result, patients may complain of less heartburn with Barrett’s esophagus. Unfortunately, this is a pre-cancerous condition: patients with Barrett’s esophagus have approximately a 30-fold increased risk of developing esophageal cancer. These patients should be followed by endoscopy.
Esophageal Cancer
If GERD is left untreated for many years, it could lead to this most serious complication – Barrett’s esophagus and esophageal cancer. In patients with chronic heartburn, an endoscopy will often be recommended to visually monitor the condition of the lining of the esophagus and identify or confirm the absence of any suspicious or pre-malignant lesions, such as Barrett’s esophagus. The preventative strategy is to treat GERD. Survival rate for esophageal cancer, at this time, is dismal.
Treatments
In many cases, infrequent heartburn can be controlled by lifestyle modifications and proper use of over-the-counter medicines.
Lifestyle and Dietary Modifications
In order to decrease the amount of gastric contents that reach the lower esophagus, certain simple guidelines should be followed:
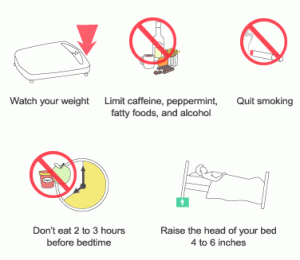
Eat small frequent meals rather than fewer large meals.
Medical Treatment of GERD
GERD has a physical cause, and frequently is not curtailed by these lifestyle factors alone. If you are using over-the-counter medications two or more times a week, your doctor may recommend evaluation for GERD and prescribe medications that reduce acid production, increase LES tone, or improve gastric emptying.
Surgical Treatment of GERD
Surgical measures to prevent reflux can be considered if other measures fail or complications occur such as bleeding, recurrent stricture, or Barrett’s esophagus (abnormal transformation of cells lining the esophagus). The surgical technique improves the natural barrier between the stomach and the esophagus that prevents acid reflux from occurring. Consultation with both a gastroenterologist and a surgeon is recommended prior to such a decision. There are always new treatments and possibilities looming on the horizon.
Any time an internal body part pushes into an area where it doesn’t belong, it’s called a hernia. The hiatus is an opening in the diaphragm — the muscular wall separating the chest cavity from the abdomen. In a hiatal hernia (also called hiatus hernia) the stomach bulges up into the chest through that opening. There are two main types of hiatal hernias: sliding and paraesophageal (next to the esophagus).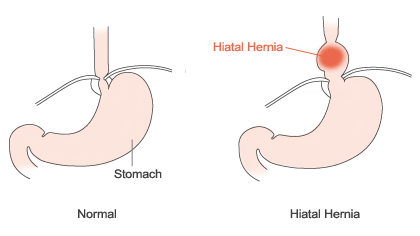
In a sliding hiatal hernia, the stomach and the section of the esophagus that joins the stomach slide up into the chest through the hiatus. This is the more common type of hernia.
The paraesophageal hernia is less common, but is more cause for concern. The esophagus and stomach stay in their normal locations, but part of the stomach squeezes through the hiatus, landing it next to the esophagus. Although you can have this type of hernia without any symptoms, the danger is that the stomach can become “strangled,” or have its blood supply shut off.
Often, people with hiatal hernia also have heartburn or acid reflux disease. Although there appears to be a link, one condition does not seem to cause the other.
What Causes a Hiatal Hernia?
Most of the time, the cause is not known. Some people develop a hiatal hernia after sustaining an injury to that area of the body; others are born with a weakness or an especially large hiatus. Increased pressure in the abdomen from coughing, straining during bowel movements, pregnancy and delivery, or substantial weight gain may contribute to the development of a hiatal hernia. In addition to the increased occurrence in people over fifty, hiatal hernias also occur more often in overweight people (especially women) and smokers.
How Is a Hiatal Hernia Diagnosed?
A hiatal hernia can be diagnosed with a specialized X-ray study that allows visualization of the esophagus (barium swallow) or with upper endoscopy.
How Are Hiatal Hernias Treated?
Most people do not experience any symptoms of their hiatal hernia so no treatment is necessary unless there are symptoms of acid reflux disease. However, the paraesophaeal hernia (when part of the stomach squeezes through the hiatus) can cause the stomach to be strangled so surgery is usually recommended.
About Swallowing Problems
Swallowing disorders, also known as dysphagia, have been found to occur in five to 15 percent of the population. It is estimated that 15 million Americans have discomfort or difficulty swallowing.
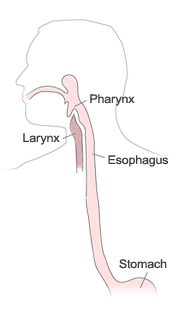 Drinking a glass of water, or eating a meal are simple, everyday activities that can give us great pleasure and at the same time be so automatic that we take them for granted. However, normal swallowing of food and liquid requires a great deal of coordination of a large number of muscles in the mouth, throat (pharynx) and esophagus.
Drinking a glass of water, or eating a meal are simple, everyday activities that can give us great pleasure and at the same time be so automatic that we take them for granted. However, normal swallowing of food and liquid requires a great deal of coordination of a large number of muscles in the mouth, throat (pharynx) and esophagus.
Normal swallowing is safe because the larynx or entrance to the windpipe is closed as food passes. The food is normally moved efficiently through the mouth and throat with little trace of food left behind. When larger amounts of food are swallowed at a time, the swallow takes longer and the muscles of the mouth and throat work simultaneously. At times we hold our breath to protect the windpipe as we prepare to swallow. While normal swallowing may change at times depending on how much or what type of food is swallowed, the safety and efficiency of swallowing do not change.
Signs and symptoms of swallowing disorders include:
- Coughing or choking when eating or drinking
- Changes in voice quality when eating or drinking
- Food or liquid leaking from the mouth or getting stuck in the throat
- Extra time needed to eat or drink
- Recurrent pneumonia
- Weight loss
- Dehydration
Difficulty swallowing may eventually result in poor nutrition or dehydration and can lead to pneumonia or chronic lung disease.
The act of swallowing is divided into three phases:
1. The oral or mouth phase — moving food or liquid into the throat.
2. The pharyngeal or throat phase — squeezing food down the throat and closing the airway to prevent choking.
3. The esophageal phase — relaxing and tightening the openings at the top and bottom of the esophagus and squeezing food through the esophagus into the stomach.
Swallowing problems (dysphagia) can be grouped into two categories:
Oropharyngeal Dysphagia
These swallowing problems happen before food reaches the esophagus and may result from neuromuscular disease or obstructions. Patients experience difficulty starting a swallow; food goes down the wrong pipe; or there is choking and coughing. This may result in poor nutrition or dehydration, aspiration (which can lead to pneumonia and chronic lung disease) or embarrassment in social situations that involve eating. Conditions that may cause oropharyngeal dysphagia include Alzheimer’s disease, Lou Gehrig’s disease, brain injury, cerebral palsy, multiple sclerosis, muscular dystrophy, Parkinson’s disease, spinal cord injury, stroke, Zenker’s diverticulum, cervical osteophytes or other obstructions.
Esophageal Dysphagia
These swallowing problems originate in the esophagus. Food or liquids “stick” in the chest or throat and sometimes come back up. Causes include mucosal rings, esophageal cancer, esophagitis, gastroesophageal reflux disease (GERD) and esophageal-motility disorders.
Individuals with dysphagia should seek a thorough examination because swallowing problems may indicate cancer of the head, neck or esophagus.
Your Digestive Tract
Acid is produced by cells in the stomach. Acid aids in digestion, helps the intestine with digestion and absorption of minerals and helps to kill food borne bacteria from entering the digestive system. Your stomach lining is a remarkably resilient membrane. A layer of mucus protects the stomach from its own acids. Similar mechanisms protect the duodenum (the first part of the small intestine). Some of the gastric juices involved in the digestive process are as toxic as car battery acid, so a healthy stomach and intestinal lining play a key role in your overall health.
Peptic Ulcer Disease
Peptic ulcer disease occurs when the stomach acid penetrates the stomach or intestinal lining and causes ulcers, an often painful sore in the lining. An estimated 4 million Americans have peptic ulcer disease, and one in 10 patients will experience the disease during his or her lifetime.
When a type of bacteria called Helicobacter pylori (H. pylori) infects your stomach lining by living in or on it, it can cause an ulcer in the stomach or duodenum. The ulcer can cause abdominal pain and, in some cases, bleeding.
Untreated, the ulcer can literally create a hole in the stomach or intestinal lining (perforation). Chronic inflammation from an ulcer can cause stomach tissue swelling and scarring. Over time, this scarring may close the outlet of the stomach, preventing food from passing into the small intestine and causing vomiting and weight loss. In severe cases, ulcer complications can lead to death.
Most ulcers are associated with an infection with a bacteria called H. pylori. Ulcers are not caused by eating spicy foods or stress. It is not known how the H. pylori bacteria is transmitted, but it may spread from person to person through fecal-oral or oral-oral routes. It may also be transmitted by contaminated water sources.
Another common cause of peptic ulcer disease is the regular use of pain medications called non-steroidal anti-inflammatory drugs (NSAIDs), which include aspirin, ibuprofen, naproxen, ketoprofen, meloxicam and celecoxib. People typically take NSAIDs to reduce pain and inflammation. Frequent or longterm use of NSAIDs, especially among older persons, can increase a person’s risk of developing an ulcer. Rarely, Ulcers can form as result of hypersecretion of acid.
The most common symptom of an ulcer is a burning pain in your stomach between your breastbone and your belly button.
- You will often feel this pain when your stomach is empty, between meals generally, but it can occur at any time.
- The pain will last anywhere from a few minutes to several hours and may sometimes wake you in the middle of the night.
- Stomach pain is often reduced by food, fluids or taking antacids.
While not as common as stomach pain, other symptoms include:
- Nausea
- Vomiting
- Vomiting blood
- Blood in the stool
- Loss of appetite
- Tests for Peptic Ulcers
If you have symptoms of peptic ulcer disease, one of several tests can be done to determine if you are infected with H. pylori, such as a simple breath, blood or stool test.
An upper endoscopy is the most accurate test to determine if you have an ulcer. This procedure involves passing a small flexible tube through your mouth and into the stomach. The tube has a camera inside that can detect ulcers and allows biopsies to be taken to check for the presence of the infection. The procedure is usually performed under sedation so it is painless.
An alternative test is an X-ray test called an upper GI (gastrointestinal) series. The patient drinks contrast liquid called barium, a thick, white, milkshake-like liquid. Barium coats the inside lining of the esophagus, stomach and small intestine, and makes them visualization easier on X-rays. The radiologist will look for ulcers, scar tissue or areas where something is blocking the normal path of food through the digestive system.
Treatment for Ulcers
Treatment for H. pylori infection usually consists of taking two antibiotics (such as amoxicillin, tetracycline, metronidazole or clarithromycin), a medication that contains bismuth, and another medicine that reduces the acid in the stomach. Generally, the antibiotic therapy is given for one to two weeks.
During the treatment, alcoholic beverages and cigarettes should be avoided, as they inhibit ulcer healing. Once the medicine has eliminated the ulcer, there is a 90 percent chance that the disease is completely cured.
When is Surgery Necessary?
With proper treatment, surgery is usually not necessary. However, if an ulcer fails to heal, if there are bleeding complications, or if a perforation (hole) or obstruction in the stomach develops, surgery is usually indicated. Fortunately, surgical therapy is rarely needed because of the efficacy of medical treatment.
