There are two main types of hiatal hernias: sliding and paraesophageal (next to the esophagus).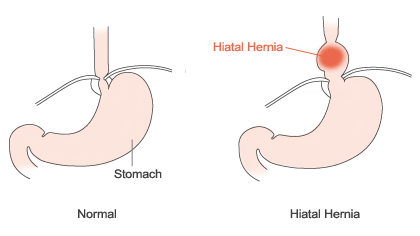
In a sliding hiatal hernia, the stomach and the section of the esophagus that joins the stomach slide up into the chest through the hiatus. This is the more common type of hernia.
The paraesophageal hernia is less common, but is more cause for concern. The esophagus and stomach stay in their normal locations, but part of the stomach squeezes through the hiatus, landing it next to the esophagus. Although you can have this type of hernia without any symptoms, the danger is that the stomach can become “strangled,” or have its blood supply shut off.
Often, people with hiatal hernia also have heartburn or acid reflux disease. Although there appears to be a link, one condition does not seem to cause the other.
What Causes a Hiatal Hernia?
Most of the time, the cause is not known. Some people develop a hiatal hernia after sustaining an injury to that area of the body; others are born with a weakness or an especially large hiatus. Increased pressure in the abdomen from coughing, straining during bowel movements, pregnancy and delivery, or substantial weight gain may contribute to the development of a hiatal hernia. In addition to the increased occurrence in people over fifty, hiatal hernias also occur more often in overweight people (especially women) and smokers.
How Is a Hiatal Hernia Diagnosed?
A hiatal hernia can be diagnosed with a specialized X-ray study that allows visualization of the esophagus (barium swallow) or with upper endoscopy.
How Are Hiatal Hernias Treated?
Most people do not experience any symptoms of their hiatal hernia so no treatment is necessary unless there are symptoms of acid reflux disease. However, the paraesophaeal hernia (when part of the stomach squeezes through the hiatus) can cause the stomach to be strangled so surgery is usually recommended.
